American National Insurance: A Business Process Management Case Study
Abstract
| Boston, MA, USA December 13, 2004 Disciplined use of BPM tools can drive impressive service improvements and transform the insurance technology environment. Business process management (BPM) is a tool with immense promise for insurance carriers because it can help address product and legacy system complexity. This report outlines American Nationals BPM strategies from 1998 through today, including its choice of Pegasystems as a BPM vendor. Efforts in the companys Health Client Service Center and Independent Marketing Organization Field Service Center are described in detail to illustrate how the work was organized and the specific results obtained. "American National exemplifies what can be achieved when the right tools are used in the right way," says senior analyst Craig Weber, author of the case study. "By taking a holistic view of business processes and how they can be supported by technology, American National has made dramatic service improvements without unplugging a bunch of back-end systems and starting over," Weber says. "The company has found a way to leverage its existing legacy infrastructure, which is a challenge that most carriers face." Dramatic Results From Applying BPM In The Health Client Service Center
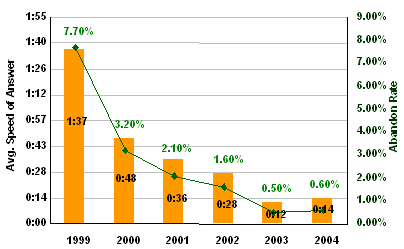
Weber notes that American National has successfully built process awareness through the company, and its cadre of "workflow architects"who design business processes and codify them using BPM software has helped facilitate and automate literally hundreds of business processes, with dramatic results. In the companys Health Client Service Center, the average speed-of-answer has been slashed from one minute 37 seconds in 1999 to 14 seconds in 2004. At the same time, the abandon rate dropped from almost 8 percent to a paltry 0.6 percent. "Its hard to overestimate the value of these improvements," Weber says. "Customer and agent satisfaction are clearly tied to the companys long-term profitability." This 31-page report contains 12 figures and six tables. A table of contents is available online. |
of Celent Communications' Life/Health Insurance research service can download the report electronically by clicking on the icon to the left. Non-members should contact info@celent.com for more information. |
|