The "Retailish" Future of Patient Collections
Abstract
A major cost shift in the healthcare market is beginning to place a significant patient collections burden on healthcare providers. Rather than collecting from a limited set of payers (health plan carriers and administrators), providers are being forced to collect from a large set of disparate consumers, with whom relationships may be relatively tenuous.
Major changes in the healthcare market are sending out strong signals that healthcare providers (hospitals, physician practices, labs) need to increasingly focus their revenue collections efforts on patients. Providers have been very slow to recognize these changes and continue to be mired in a culture where collections are not made at the point of service and where even asking for payment is done in a somewhat apologetic manner. Although by 2012, patients will account for 30% of providers’ revenue sources, the overwhelming majority of providers are not equipped to collect at the point of care. In other words, the healthcare market is arguably the most "unretail" consumer-facing industry in the US today.
However, with healthcare costs rapidly shifting to consumers, the patient collections situation has no choice but to change. As consumers constitute more and more of providers’ revenue sources, the inability to collect from those consumers is unsustainable and tantamount to provider bankruptcy. Although the presence of third party payers prevents evolution to a true retail environment, providers must adopt more aggressive, "retailish" collection methods -- those that support transparency, speed, and importantly collection/payment assurance at the point of care. This will lead to another important shift in consumer behavior and attitudes -- consumers are simply going to have to get used to a retail-like healthcare environment, where a substantial payment (or commitment to do so) is expected up front. Providers’ need for financial solvency will dictate so.
Because of this need, a new generation of patient revenue cycle management (RCM) solutions is entering the market. These solutions borrow concepts similar to those of other industries to make healthcare "retailish," improve collections, and lower process costs. Among the various functionalities offered, real time adjudication, and "right time" adjudication in concert with a payment account on file stand out in their ability to improve collections at the point of service. Whereas RTA has limitations, the "right time" adjudication approach should be able to function within the constraints of the healthcare claims processing and adjudication process.
Report highlights include the following:
- On an unweighted average, each provider location will be responsible for collecting $317,000 from consumers by 2014.
- By 2012, patient responsibilities (patient receivables) will constitute 30% of providers’ total revenues, an increase from 12% of revenues in 2007.
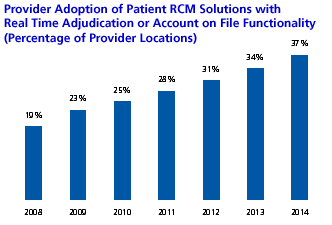
- By 2014, 37% of provider ambulatory (excluding dentists) and hospital locations will have patient RCM solutions in place that enable upfront collections/payment assurance via real-time adjudication or payment account on file functionality.
"Within this growing space, banks clearly have a role to play," says Red Gillen, senior analyst with Celent's banking group and author of the report. "By leveraging pre-existing relationships with providers, banks can serve as channel partners, wholesaling vendors’ patient RCM solutions. Conversely, banks can cross-sell products to RCM channel partners' clients. Whereas some of these bank products may be more traditional, other bank products may be highly complementary to RCM solutions. Such complementary products include merchant card acquiring, enhanced remote deposit capture/lockbox, patient financing and provider financing."
This report provides an analysis of underlying factors and trends behind the anticipated growth of patient RCM solutions. An overview of vendors in the patient RCM space is also included.
The report contains 49 pages and 17 figures and five tables. A table of contents is available online.
Members of Celent's Healthcare Banking research service can download the report electronically by clicking on the icon to the left. Non-members should contact info@celent.com for more information.

